Heart Health Month
- Maria Scuor
- Feb 15, 2024
- 8 min read

In Canada and the USA, February is the dedicated month for supporting and getting to know more about heart health. It was 60 years ago in 1964, that President Lyndon B. Johnson issued the proclamation declaring February Heart Health Month. Having a healthy heart is so important to living life well always that I thought I’d do a blog to remind us what we need to do to keep our heart ticking perfectly.
Heart disease is the second leading cause of death in Canada and the number one cause of death in the USA and world-wide. Therefore, it is important to take our hearts seriously and learn more about the diseases that impact it. Types of heart diseases are:
Coronary Artery Disease (CAD)
CAD is the most common heart disease and blockage in coronary arteries leads to less blood flow to our heart
Symptoms: chest pain called angina, shortness of breath, and if there is sever blockage of blood flow will lead to heart attack
At risk: age over 55 for men and women when in menopause, being inactive, having diabetes, family history of CAD, genetics, high blood pressure, high levels of LDL” bad” cholesterol, or low levels of HDL “good cholesterol, stress, smoking and obesity
Treatments: medication to lower blood pressure or cholesterol, life style changes of eliminating smoking, vaping or tobacco products, eating healthy, low sodium, Mediterranean diet, 30 minutes of exercise per day, limited alcohol intake, percutaneous coronary intervention or angioplasty, coronary bypass grafting
Here is a picture of what CAD looks like. Photo take from Cleveland Clinic Website

Heart Arrhythmia
Also known as dysrhythmia, is when our hearts beat abnormally. 1.5 – 5% of people have arrhythmias. Arrhythmia can start in different parts of the heart and they can be too fast, too slow or irregular.
Supraventricular arrhythmia begins in the upper part of our hearts
Atria Ventricular arrhythmia begins in the lower chamber of our hearts, the ventricles
Bradyarrhythmia and junctional rhythms happen due to our hearts conductive system
Causes can be from: heart disease, wrong electrolyte balance in blood, heart injury, infection or fever, certain medications, problems with electrical signals in our heart, diabetes, alcohol, tobacco, caffeine, exercise, high blood pressure, sleep apnea, problems with thyroid gland, anxiety, cardiomyopathy and hormone level changes
Symptoms: palpitations (feeling of skipped heartbeat or fluttering), pounding in chest, shortness of breath, chest pains, dizziness or feeling lightheaded, fainting, weakness, fatigue, blurred vision, sweating, anxiety, rapid or slow heartbeat
At risk: chances go up as we get older, can run in the family, lifestyle with too much alcohol, tobacco or recreational drugs, medical conditions, environment like pollution and heart disease
Treatments: medication such as antiarrhythmic drugs, anticoagulants, or ones that control heart rate, lifestyle changes in managing blood pressure and blood sugar, avoiding tobacco, cutting back on alcohol, avoiding caffeine, healthy weight, therapies such as cardioversion, catheter ablation or pulmonary vein isolation, pacemaker, and sometimes bypass surgery
Here is a picture of what Cardiac arrhythmia looks like. Photo take from Modern Heart and Vascular Website

Heart Valve Disease
Our hearts have four valves (Mitral, Tricuspid, Aortic and Pulmonary) and sometimes they don’t open and close the right way.
Types of heart valve disease include:
Stenosis – valve flaps become too thick or stiff and join together making the opening narrow that blood flow is impacted
Regurgitation – when valves don’t close properly and cause blood to leak backward
Prolapse – valve becomes stretched and floppy and bulges like a parachute, it leads to regurgitation
Atresia – valve isn’t formed as solid tissue blocks the blood flow between chambers, usually affect pulmonary valve
Congenital Heart Valve Disease – some people are born with this
Heart valve disease is very common problem and medication can help with blood flow problems due to a heart valve not working right. But sometimes medication isn’t enough and it would need to be repaired.
Symptoms: shortness of breath at rest, lying down or active, fatigue, dizziness, chest pains, swelling of ankles and feet, fainting and irregular heartbeat
At risk: older age, infections such as rheumatic fever or blood infections, heart attacks or some type of other heart disease, high blood pressure, high cholesterol and diabetes
Treatment: medication such as beta-blockers, digoxin and calcium channel blockers, medication to control blood pressure, surgery to repair the valves, surgery to replace a valve, balloon valvuloplasty which is non-surgical procedure
Here are photos heart chambers and valves taken from Mayo Clinic Website

Pericarditis and Myocarditis
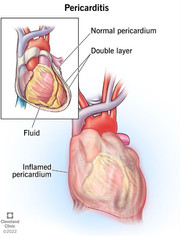
Pericarditis is the inflammation of the pericardium sac that holds our hearts and is often caused by a virus, inflammatory diseases such as lupus or rheumatoid arthritis, or injury to your pericardium. Pericarditis can often follow after open heart surgery.
Symptoms: sharp stabbing chest pain which can get worse with coughing, swallowing, taking deep breaths or laying down, pain in back, neck or shoulder, dry coughs, trouble breathing when lying down, palpitations, anxiety or fatigue, fever, swelling legs and feet
At risk: men and women get it however men between 20 and 40 years of age are more likely to be affected than older people. 20-30% of people who undergo treatment have a chance of developing the condition again, if you have had a heart attack, kidney failure, heart surgery, cancer and tuberculosis
Treatment: Medication for pain and inflammation, pericardiocentesis procedure to drain the fluid, and if constrictive pericarditis (walls of the fluid-filled pouch around the heart becomes to thick or stiff) exists then pericardiectomy surgery is performed. This removes part or all the pericardium from the heart. Thankfully we can live without the pericardium
Myocarditis is the inflammation of the heart muscle and most often caused by: the flu, many types of viruses, bacteria, rheumatic, fever, lupus, and rarely fungi.
Symptoms: chest pain or feeling of tightness, shortness of breath, tiredness, palpitations, irregular heartbeat, feeling light-headed or faint, flu symptom, fever, headaches, sore throat, and rarely swelling of hands, legs, ankles or feet, pain in abdomen, no appetite and not able to exercise
At risk: young adult, however people of all ages can get it, your body doesn’t react well to inflammation, you drink too much alcohol, are on dialysis, have heart device implanted, radiation, diabetes, HIV/AIDS, cancer treated with certain medicines, eating disorder, kidney disease, or chest injury
Treatment: painkillers or analgesia for chest pain, inflammation medication, antibiotics, rest, plenty of fluids, pacemaker, left ventricular assist device or a donor heart
Unfortunately, it is very hard to avoid many of the things that cause myocarditis therefore prevention is hard. It is important to wash hands often, stay healthy, keep up with flu vaccines, limit alcohol intake and don’t take prohibited drugs
Here is a photo of Pericarditis taken from Cleveland Clinic Website as well as photo of Myocarditis from Cleveland Clinic Website
Cardiomyopathy
This is when the myocardium heart muscle stiffens, gets enlarged or thickened and causes scar tissue. As a result, cardiomyopathy disease can’t pump blood effectively to the rest of our body. In time, the heart will weaken and cause heart failure. There are many types of cardiomyopathies but there four main ones:
Dilated: one of the ventricles of the heart is enlarged, more common in males, and most common cardiomyopathy in children, it occurs at any age and isn’t inherited
Hypertrophic: it is when the heart muscle is thickened, often presents in children or early adulthood, can cause sudden death, often inherited, may not have symptoms. It is believed to be the most common inherited or genetic heart disease
Arrhythmogenic: causes irregular heartbeat or rhythms, mostly in males, often inherited
Restrictive: heart muscle is stiff, scarred or both and is the least common
The most common inherited cardiomyopathy, hypertrophic, affects about 1 in 500 people in the world. Other genetic types occur in 1 in 2,000 or 2,500 people.
Symptoms: shortness of breath, trouble breathing, fatigue, swelling in the ankles and legs, irregular heart beat, palpitations or fainting
At risk: diabetes, high blood pressure, high cholesterol, high triglycerides, BMI higher than 25
Treatment: treatments don’t cure the condition but can help with the symptoms and slow the disease’s progression. Depending on the cause, certain medications can improve blood flow and manage symptoms. Lifestyle changes such as eating healthy with less fat and salt, getting regular exercise, reducing stress level, sleeping well, avoiding tobacco or alcohol, and maintaining the appropriate weight. Devices may be added to your body to treat irregular heartbeat or improve blood flow. If symptoms are severe, surgeries may be needed, which may include a heart transplant
Here is a picture of what Cardiomyopathy looks like. Photo take from Cleveland Clinic Website

Congenital Heart Disease (CHD)
Congenital means that you are born with the condition at birth. Therefore, this heart disease means you have one or more issues with your heart at time of birth. Sometimes these can be detected before birth, soon after birth or anytime throughout life. Problems can be a hole in the heart, issues with blood vessels and problems with heart valves.
There are many types of CHD and symptoms and treatment depends of the type of defect as well as the severity. A diagnosis of congenital heart disease means lifelong medical care, which include regular checkups, medication or surgery.
Symptoms: cyanosis (blueish skin, lips, nails), sleepiness, trouble breathing, fatigue, heart murmur, poor blood circulation, weak pulse or pounding heart and fast breathing
At risk: this type of heart disease happens when the fetal heart doesn’t develop correctly in the uterus. It isn’t fully understood why this happens but may be related to abnormal chromosomes or genetics, drinking or smoking during pregnancy, or illnesses in mother during pregnancy
Treatment: some CHD cases may heal by themselves, others may remain but don’t need treatment, while others must be treated as soon as the baby is born. Treatments may include:
Medications – to help heart work more efficiently or to manage blood pressure
Catheter – procedure to place a plug into the defective heart
Closing device – nonsurgical procedure to close the defect
Heart health month is an opportunity for us to learn about how we can reduce our risk by eliminating what we have control over. Here are a few things we can do:
Eating healthy and balanced: low-fat, high-fibre, 5 portions of fruit and vegetables per day, whole grains
More physically active: 30 minutes of regular exercise per day will make our hearts circulate more efficient, lower cholesterol and keep our blood pressure at a healthy level. Walking, swimming, aerobic exercise and even dancing makes our heart work harder and keeps it healthier
Keep a healthy weight: our doctors are able to give us our ideal weight in relation to height and build. Also we can calculate our body mass index (BMI) which measures body fat based on height and weight that applies to adult men and women
Stop smoking: giving up smoking reduces risk of developing CHD. It also is a major risk factor for developing atherosclerosis
Reduce alcohol consumption: researchers have recognized that alcohol consumption can directly damage heart muscle cells. Reducing the amount of alcohol we drink should see an improvement in blood pressure. Avoid binge drinking as this increases risk of heart attack
Keep blood pressure under control: eating healthy, exercising regularly and if needed taking medication to lower blood pressure will help keep our blood pressure under control
Keep diabetes under control: if you have diabetes, you have a higher chance of getting CHD. Lower your risk by keeping active and controlling your weight. Make sure blood pressure, cholesterol and sugar levels are checked regularly
Take medications: if you have CHD, you may have prescribed medications to help with they symptoms and developing further problems. If you don’t have CHD then ensure you always check with your doctor to make sure your cholesterol, blood pressure, diabetes is regularly tested so you can have prescribed drugs help prevent developing heart-related problems
Find the positives in everything you do because there is always a silver lining. Challenges are part of life and if we take them as a learning opportunity, life is better. Take time to get outside and breath the incredible air we have and see the beauty that the world has to offer.
Live life well always by learning something new each day to make you healthier and happier.






Comments